Achilles Tendinopathy: Causes, Symptoms, Treatment, and Specific Considerations in Athletes
- Ghenadie Cislari

- Mar 1
- 3 min read
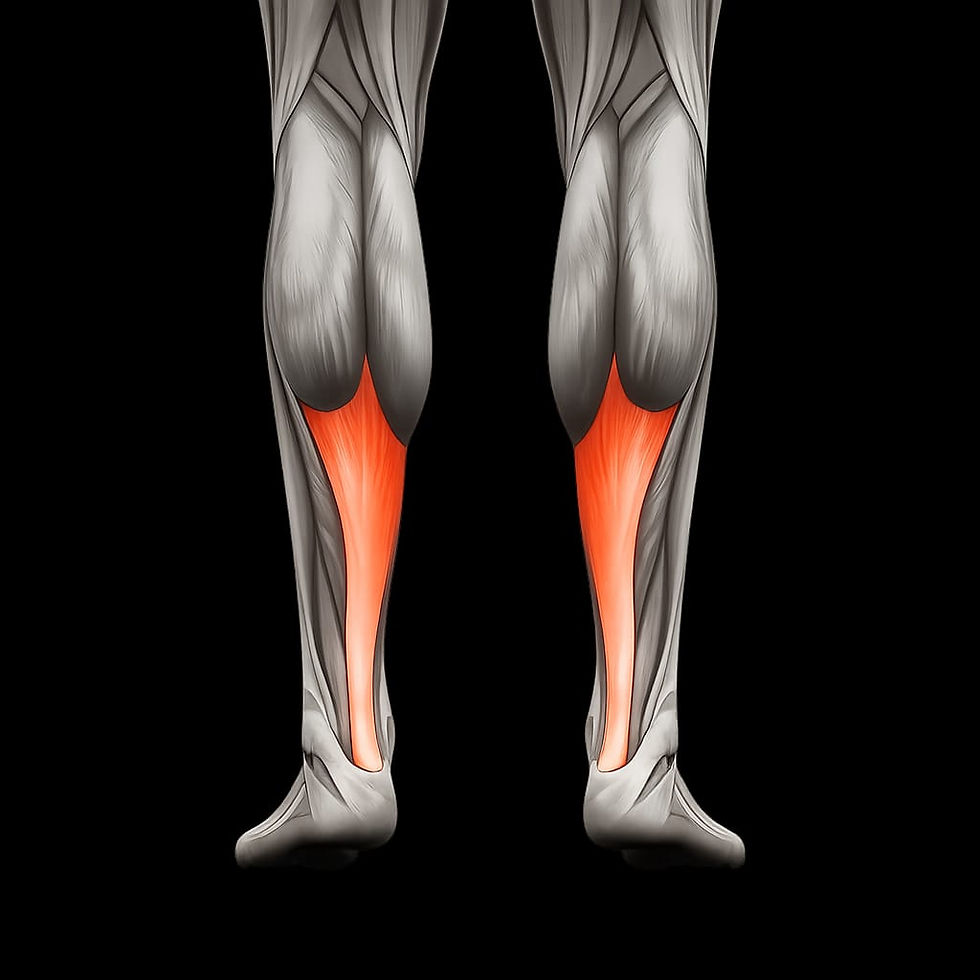
What Is Achilles Tendinopathy?
Achilles tendinopathy refers to painful and degenerative changes within the Achilles tendon. Unlike classic inflammation, this condition typically results from chronic overload on the tendon, rather than an acute inflammatory response.
The Role of the Achilles Tendon
The Achilles tendon is the strongest tendon in the human body. It connects the calf muscles to the heel bone and is essential for several movements, including:
Walking
Running
Jumping
Acceleration and changing direction
When the mechanical load on the tendon exceeds its ability to adapt, microdamage occurs. This can cause thickening of the tendon, structural alterations, and discomfort.
Main Causes of Achilles Tendinopathy
Sudden increase in training volume
Running on hard surfaces
Wearing inappropriate footwear
Limited ankle mobility
Weakness in the calf muscles
Excess body weight
Sedentary work combined with bursts of high-intensity activity
Ultimately, Achilles tendinopathy is a problem of load management.
Symptoms
Pain located 2–6 cm above the heel bone
Morning stiffness
Tendon thickening
Tenderness when palpated
Increased pain after activity
It is important to note that if pain decreases during warm-up but returns after exercise, this signals continued overload of the tendon.
Types of Achilles Tendinopathy
Mid-portion tendinopathy: The most common type, occurring 2–6 cm above where the tendon inserts into the heel bone.
Insertional tendinopathy: Located at the attachment of the tendon to the heel bone.
Treatment approaches are tailored slightly depending on the specific type involved.
Diagnosis
Clinical examination
Functional testing
Ultrasound imaging
MRI when necessary
For most cases, a comprehensive clinical assessment is sufficient for diagnosis.
Achilles Tendinopathy in Athletes
Why Are Athletes at Higher Risk?
In athletes, the Achilles tendon is exposed to repetitive, explosive loading, accelerations and sudden stops, high plyometric demands, and large running volumes. Insufficient recovery also contributes to increased risk. This condition is especially common in:
Football players
Track and field athletes
Basketball players
CrossFit athletes
Tennis players
Common Mistakes in Athletes
Continuing to train or compete despite pain
Relying solely on nonsteroidal anti-inflammatory drugs (NSAIDs)
Performing aggressive stretching
Returning to play prematurely
Neglecting structured strength training
Pain that "warms up" during activity does not indicate that the tendon has healed.
Modern Treatment Approach
❌ Complete rest is not recommended
❌ Topical treatments and medications alone are inadequate
❌ Ignoring symptoms increases the risk of rupture
✔ Load management is essential
✔ Isometric exercises help modulate pain
✔ Eccentric loading is beneficial
✔ Heavy slow resistance training aids recovery
✔ Gradual progression with plyometric exercises is advised
✔ Correcting biomechanical issues is important
✔ Weight management where needed
✔ Adjunctive physiotherapy modalities can support recovery
Controlled and progressive loading of the tendon is necessary for healing, rather than complete rest.
Return to Play Criteria
Returning to sport is appropriate when:
Morning stiffness is absent
No tenderness is present when palpating the tendon
The athlete can perform 20–25 single-leg heel raises without pain
Plyometric exercises are tolerated without symptoms
Recovery Timeline
Mild cases usually recover in 4–6 weeks
Chronic cases may require 8–12 weeks
If overload is left untreated, there is a risk of partial or complete tendon rupture
The biology of tendon adaptation cannot be rushed; proper guidance is essential for recovery.
When to Seek Urgent Medical Attention
Sudden "pop" in the heel area
Inability to stand on tiptoe
Sudden, sharp increase in pain
These signs may indicate an Achilles tendon rupture and warrant immediate medical evaluation.
Key Takeaway
Achilles tendinopathy is not a minor strain that will simply disappear on its own. It is a warning sign that mechanical load is exceeding tissue capacity. Successful management requires a systematic progression, patience, and intelligent control of training loads.




Comments